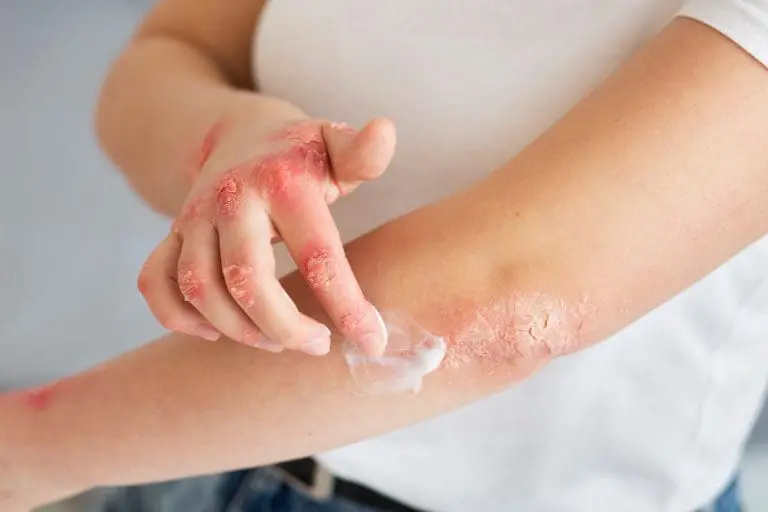
1. What is the prognosis of atopic dermatitis?
Tendency to improve after 3-7 years and puberty. In 25% of cases, it persists after the age of 25, with eczema changes becoming more localized on the limbs and neck. In 3% of cases, erythroderma develops at the beginning.
The following prognostic criteria can assist the attending physician in assessing the development of the disease.
Pessimistic:
- early onset of the disease
- presence of severe itching
- chronic-recurrent course
- other atopic manifestations
- xerosis
- frequent infections
- erythroderma
- pronounced characteropathy
Optimistic:
- late start
- seasonal dependence
- localized skin changes
- resistance to infections
2. What are the complications of atopic dermatitis?
- infection with the vaccine ( eczema vaccinatum) or herpes viruses (eczema herpeticum)
- infections with human papillomavirus and molluscum contagiosum occur with more disseminated lesions that are difficult to eliminate
- 3% of patients develop atopic erythroderma
- complications from topical corticosteroids with long and incorrect use – skin atrophy, stretch marks, pyodermas, viral infections, etc.
- tachyphylaxis to topical corticosteroids occurs if they are not used correctly
3. What are the drug treatment regimens?
Anti-inflammatory agents – topical corticosteroids reduce the inflammation of eczematous lesions. The use of ointments provides hydration. White petroleum jelly is useful for avoiding potential sensitization to preservatives used in creams.
- Hydrocortisone (Locoid lipochrome) – suppresses inflammation by inhibiting the migration of polymorphonuclear leukocytes and reducing capillary permeability. A weakly potent corticosteroid and is the drug of first choice. A thin film is applied to the affected area 2 to 4 times daily until a satisfactory response is achieved
- Betamethasone (Diprosone, Betnovate) – suppresses inflammation by inhibiting the migration of polymorphonuclear leukocytes and reducing capillary permeability. It affects the production of lymphokines and inhibits Langerhans cells. A potent corticosteroid and is used in psoriasis resistant to low potency corticosteroids. A thin film is applied 2/4 times a day until the effect is achieved.
- Hydroxyzine (Atarax, Neurolax) – antagonist of peripheral H1 receptors. It inhibits the action of histamine in the subcortical department of the CNS. Antihistamine with sedative action. 25-100 mg PO every 4-6 h; not to exceed 600 mg/d. In children, 2 mg/kg/d PO divided into 6-8 h.
- Diphenhydramine (Benadryl N) – for symptomatic relief of symptoms caused by released histamine. 25-50 mg PO every 6-8h; not to exceed 400 mg/d. In children, 5 mg/kg/d PO divided by 6 h; not to exceed 300 mg/d.
Immunomodulators – for the treatment of severe forms of atopic dermatitis, in which conventional therapy has no effect.
- Cyclosporin (Sandimmune) – has an effect on various diseases, especially psoriasis. It works by inhibiting the production of cytokines and interleukins by T-cells. Like tacrolimus and pimecrolimus, cyclosporine binds to macrophilin and inhibits calcineurin, which is a calcium-dependent enzyme and inhibits the transcription of cytokines, particularly IL-4. Treatment is discontinued if there is no response after 6 weeks. 2 mg/kg/d po in two divided doses; if no improvement is noted after 1 month, the dosage can be gradually increased; not to exceed 5mg/kg/d; when the skin lesions improve, the dose is reduced by 0.5-1 mg/kg/day/month; a minimum maintenance dose is required. In children 3-5 mg/kg/d po.
- Methotrexate – inhibits DNA synthesis in tissues by antagonizing folic acid. Systemic therapy after phototherapy is unsuccessful. It has an immunosuppressive effect. 7.5 mg test dose; CKD and liver function control after 1 week; if laboratory results are normal, therapy can be continued; 2.5-10 mg PO every 12 hours for 3 doses/week (average dose 10-25 mg PO/IM/IV weekly) until the desired response is achieved; not to exceed 30 mg/week; the dose can be given once a week. Not recommended for children.
- Tacrolimus (Protopic) – a local immunomodulator that inhibits the production of cytokines by T-lymphocytes. Studies have shown excellent results against placebo and hydrocortisone 1%. For adults 0.03-0.1% ointment and 0.03% ointment for children. A thin layer is applied to the affected skin twice a day; treatment is continued for 1 week after symptoms subside.
Antibiotics – cloxacillin or cephalexin are used to treat clinically apparent staphylococcal infection. If the infection is streptococcal, cephalexin is preferred.
- Cephalexin (Keflex) – first-generation cephalosporin; suppresses bacterial growth by inhibiting the synthesis of the bacterial wall; bactericidal action against rapidly growing microorganisms; used for the treatment of skin infections or prevention of minimal interventions. Suspensions 125 mg/5 mL and 250 mg/5 mL. 1-4 g/d PO every 6 hours, in children 25-50 mg/kg/d PO every 6 hours.
- Cloxacillin – to treat infections caused by penicillinase-producing staphylococci. It can be used as initial therapy for suspected staphylococcal infection. 250-500 mg PO every 6h. In children <20 kg: 50-100 mg/kg/d PO divided every 6h>20 kg: 250 mg PO every 6h
4. What is the treatment for atopic dermatitis?
The therapy includes a complex of measures related to regime, diet, hygiene care, and household habits for restful sleep and photoprotection.
The disease is treated on an outpatient basis, but in the stages of exacerbation, inpatient treatment may be required.
Moisturizing the skin:
- frequent oil baths (1 spoonful of oil added to the bath water) for 5-10 minutes. The body is left wet after the bath. The oil or emulsion does not allow water to evaporate into the environment.
- patients are advised to apply an emollient, e.g. petroleum jelly all over the body while wet to prevent water from evaporating and to absorb through the stratum corneum.
- local corticosteroids – use of ointments is preferred for dry and lichenified skin. AD patients may develop a contact allergy to components of topical agents. Allergy to hydrocortisone is also present and the frequency k is increasing. Allergy to cream preservatives is more common, which is not characteristic of ointments. Initial therapy includes hydrocortisone 1% 3 times a day for facial lesions and folds. Moderately potent corticosteroids (triamcinolone or betamethasone valeriate) are applied 3 times a day to lesions on the body until an effect is achieved.
- UV exposure – UV-A, UV-B or a combination of both; psoralen plus UV-A (PUVA) may be beneficial.
- antihistamines – used to relieve itching, but are not effective without other treatment.
- antibiotics – used to treat superimposed staph infection. Cloxacillin or cephalexin are used. For resistant strains, penicillin and clindamycin can be used in combination. Laboratory isolation of S. aureus is not indicative of clinical infection, as staphylococcal organisms routinely colonize the skin of AD patients.
- other means – thymopentin, interferon-gamma, glandular, Chinese herbs have little significance in practice.
Tacrolimus (topical FK506) is an immunomodulator licensed in Japan and the United States. Studies show excellent results compared to placebo and hydrocortisone 1%. Absorption is low and side effects such as skin atrophy are not observed. Sometimes burning is observed after application, which can be reduced by applying the medication only on dry skin. This effect usually subsides after 2-3 days.
In patients with a severe course of the disease and in adults, methotrexate and cyclosporine can be used. Cyclosporine is more effective, but relapses occur quickly after stopping it. Monitoring of renal function and hypertension is required.
Diet – avoid foods that provoke acute allergic reactions (urticaria, anaphylaxis). Allergic reactions are most often caused by peanuts, eggs, seafood, soy, milk, and chocolate.
5. What is the differential diagnosis of atopic dermatitis?
In terms of differential diagnosis, the following diseases are taken into consideration:
- contact allergic dermatitis
- contact irritant dermatitis
- lichen simplex chronicus
- eczema nummular
- psoriasis vulgaris
- scabies
- tinea
- seborrheic dermatitis.
Atopic dermatitis is sometimes difficult to distinguish from other causes of dermatitis. In the neonatal and nursing period, the greatest difficulty is the differentiation from seborrheic dermatitis. In atopic dermatitis and seborrheic dermatitis, crustae lactose (milk crusts) are observed, which in seborrheic dermatitis are oily and yellowish. Xerosis and severe itching are not characteristic of seborrheic dermatitis. The latter develops immediately after birth, while atopic dermatitis begins in the third month. The two diseases must be differentiated from psoriasis.
Scabies (scabies) present as a highly itchy exanthema. Other family members are also itchy. Areas of concern are humid and warm areas. In infants, palms and soles are affected. The face is free of pathological processes and the skin is not dry.
Nickel contact allergic dermatitis in children is difficult to distinguish from AD. Localization of the plaques (under nickel buttons on clothes) helps with the diagnosis, although contact allergy can spread to other areas of the body. Dry skin and facial involvement are rare. AD usually starts earlier.
Children with severe itching and generalized dermatitis should be examined for congenital immunodeficiency diseases (Job’s syndrome, Wiskott-Aldrich, etc.) and phenylketonuria.
Mycosis of the smooth skin usually occurs with a single plaque, but if misdiagnosed and treated with topical corticosteroids, it causes disseminated dermatitis.
6. How is atopic dermatitis diagnosed?
Williams et al . give the following diagnostic criteria.
patients with pruritus
patients with 3 or more of the following symptoms :
- involvement of skin folds – cubital area, popliteal fossa, or neck
- history of asthma or hay fever, as well as family history
- history of dry skin in the past year
- disease onset before 2 years of age (not used for children under 4 years of age)
In 1980, Hanifin and Rajka proposed criteria for the diagnosis of atopic dermatitis. These include numerous secondary criteria such as Hertoghe’s sign (lateral drooping of the eyebrows), the Dennie-Morgan fold (an additional fold under the lower eyelid), and other signs. Many authors question the validity of these secondary criteria.
- laboratory tests are rarely necessary. Allergy testing and the radioallergosorbent test (RAST) are of little importance. Wiskott-Aldrich syndrome is ruled out by PKC.
- assessment of cellular immunity to exclude immunodeficiency syndromes.
- mycological examination – native microscopy of scraped skin material with 30% KOH to rule out tinea
- histological examination – the biopsy is non-specific and shows evidence of acute, subacute or chronic dermatitis
7. What is the clinic for atopic dermatitis?
Continuous itching and dry skin are the main symptoms. Itching may not be noticeable in the first few weeks of life, but parents notice scratching marks by 3 months. Physical examination revealed xerosis (dryness), lichenification, and eczematous lesions. The latter change their localization and morphology with age:
- infancy and early childhood – newborn children are born with xerosis or it develops in the neonatal period. Xerosis often involves the entire body, leaving the diaper area unaffected. In newborns, the lesions develop in the area of the folds (cubital and popliteal). They are erythematous and exudative. After a few weeks, the lesions are localized on the cheeks, forehead, and extensor surface of the lower limbs, where erythematous scaly (eczema) plaques are observed. The lesions may not be as exudative as in the later phase and limited crusting is present. The scalp is dry and scaly. The capillitium area is often involved in pruritic scaly dermatitis, which must be differentiated from seborrheic dermatitis. Lichenification is not characteristic of this period.
- childhood – generalized xerosis. Eczema and exudative lesions. The pallor of the face with erythema and desquamation around the eyes is common. Flexor folds – cubital and popliteal – are most often affected. Excoriations and crusts are common symptoms.
- adults – lesions become more diffuse on an erythematous basis. The face is often affected. Skin dryness and lichenification are pronounced. A brownish ring around the neck is typical, which is not always present.
8. What is the etiology and pathogenesis of atopic dermatitis?
A genetic defect localized to chromosomes 11q13 or 5q31 and these data must be confirmed. There is often a familial association with AD.
Laboratory findings suggest defects in TH2 cell function, leading to increased production of IL-4 and IgE. Excess IL-4 leads to reduced levels of interferon и. The cells react with antigens from the environment and produce a large amount of IgE.
Serum histamine and its release from cells, which is the result of mast cell degranulation due to antigen-antibody reactions, are increased.
Defects in the production of lipids (ceramides) by the stratum corneum lead to skin dryness and increased transepidermal water loss. Disorders in prostaglandin metabolism are also involved. Xerosis of the skin allows easy penetration of antigens through the skin, causing an abnormal interleukin response.
The skin of patients with atopic dermatitis is colonized with S . Aureus, which exacerbates the disease, but the condition can be worsened by any other skin (Pityrosporum, Candida, Trichophyton) or systemic infection.
Allergens from the environment exacerbate the disease:
- contact irritants (soaps, solvents, woolen clothes, perfumes, etc.) reduce the barrier functions of the epidermis and cause an inflammatory reaction. aeroallergens (house mites, pollen, etc.) induce peripheral eosinophilia and elevated serum IgE levels.
- food allergens are blamed in 1/3 to Ѕ of children with atopic dermatitis. The most common food allergens are eggs, soy, milk, wheat, fish, shellfish, and peanuts, which together account for about 90% of food-induced cases of atopic dermatitis in double-blind, placebo-controlled studies. Food allergy subsides around 1 year of age, and it is not necessary to follow restrictive diets for a long period.
- stress triggers atopic dermatitis at sites of activated cutaneous nerve endings via substance P, vasoactive intestinal peptide (VIP), or the cyclic adenosine monophosphate (cAMP) system
9. What is atopic dermatitis?
Atopic dermatitis is a genetically determined chronic-relapsing eczema disease, which is the earliest manifesting component of the atopic symptom complex, which includes manifestations from the respiratory, digestive, and CNS systems, manifesting as bronchial asthma, vasomotor rhinitis, urticaria, constipation, migraine, and atopic characteropathy.
- frequency – they affect up to 9.9% of inpatients treated and 7.3% of outpatients examined children with skin diseases in KDV-Sofia. AD patients make up about 0.8-1.0% of the Bulgarian population.
- race – the disease is distributed throughout the world, but is more common in northern regions, affecting all races.
- gender – men are more often affected by vernal and atopic conjunctivitis, compared to women.
- age – atopic dermatitis occurs at any age, but it most often begins during infancy, around 2-6 months. 75% of individuals have improvement by 10-14 years of age. 25% of patients continue to have relapses for the rest of their lives. The manifestations of the disease vary depending on age.
- obscurity – the disease is not life-threatening.
The material is informative and cannot replace consultation with a doctor. Before starting treatment, you must consult a doctor.